How to Recognize the Symptoms of Allergic Conjunctivitis and Seek Treatment
Categories: HEALTH
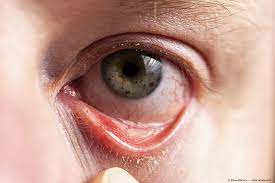
An allergic reaction to certain things, like pollen, pet dander, dust mites, or particular drugs, can result in the eye illness known as allergic conjunctivitis. It's critical to identify allergic conjunctivitis symptoms and get the right care.
The eye gets inflamed and painful. The body releases histamine and other active compounds through mast cells as a result of the overactive immune system, which causes symptoms. The nerve endings become irritated as the blood vessels dilate or expand. The end outcome is an increase in tear production. Conjunctivitis that is allergic differs from conjunctivitis that is infectious. There are various causes.
Here are some steps to help you:
1. Understand the symptoms: Allergic conjunctivitis typically affects both eyes and may include the following symptoms:
a. Redness and itching in the eyes
b. Watery or teary eyes
c. Swelling and puffiness around the eyes
d. Burning or stinging sensation
e. Sensitivity to light
f. Stringy discharge from the eyes
g. Blurred vision (rare)
2. Identify triggers: Pay attention to potential triggers that could cause your allergic conjunctivitis. Common triggers include pollen, mold spores, pet dander, dust mites, certain cosmetics or eye drops, and certain medications.
3. Seek medical advice: If you suspect you have allergic conjunctivitis, it's important to consult a healthcare professional, such as an ophthalmologist or allergist. They can evaluate your symptoms, perform necessary tests, and provide an accurate diagnosis.
4. Receive treatment recommendations: Based on the severity of your symptoms and the underlying cause, your healthcare provider may recommend one or more of the following treatments:
a. Artificial tears: Over-the-counter lubricating eye drops can help relieve dryness and wash away allergens.
b. Antihistamine eye drops: These prescription or over-the-counter eye drops help reduce itching and redness.
c. Mast cell stabilizers: These eye drops prevent the release of histamine and can help control symptoms.
d. Nonsteroidal anti-inflammatory drugs (NSAIDs): These eye drops can reduce inflammation and relieve symptoms.
e. Oral antihistamines: In some cases, your healthcare provider may prescribe oral antihistamines to alleviate systemic allergy symptoms.
5. Avoid triggers: Take steps to minimize your exposure to allergens, such as:
a. Keep windows closed during high pollen seasons.
b. Use air purifiers or filters to reduce indoor allergens.
c. Regularly clean bedding, carpets, and curtains to minimize dust mites and pet dander.
d. Avoid rubbing your eyes, as it can worsen the symptoms.
6. Follow up: If your symptoms persist or worsen despite treatment, or if you experience any changes in your vision, consult your healthcare provider for further evaluation and guidance.
Causes of allergic conjunctivitis:
When the immune system overreacts to a chemical, an allergic reaction occurs. Most people do not respond to dust, pollen, and other things in this way, but some people are more sensitive.
Most frequently, the following allergens induce allergic conjunctivitis:
1. Pollen, which causes hay fever
2. Animal fur
3. Ointments
4. Cosmetics
5. Dust mites
Types of allergic conjunctivitis:
Different forms of allergic conjunctivitis exist.
1) Seasonal allergic conjunctivitis or allergic rhinoconjunctivitis: In nations with chilly winters, pollen is the allergen that causes conjunctivitis the most frequently. There may probably be additional symptoms, such as sneezing, an itchy, clogged, or runny nose, as well as itchy and watery eyes, if conjunctivitis is brought on by pollen. Hay fever is another name for allergic rhinoconjunctivitis or seasonal allergic conjunctivitis. Typically, it takes place throughout the spring and summer. Plants are currently covered in pollen, especially grass, trees, and flowers. Early in the autumn, some people have symptoms.
2) Contact conjunctivitis: The condition is sometimes referred to as contact dermatoconjunctivitis, and its symptoms are typically brought on by eye drops, cosmetics, or other chemicals that irritate conjunctiva in sensitive individuals. An allergic reaction occurs when these compounds are in contact with you. Some individuals are hypersensitive to certain drugs. Typically, symptoms appear 2 to 4 days after the chemical contacts the eyes.
3) Giant papillary conjunctivitis: Wearing contact lenses frequently has this effect. Contact lenses can make some individuals uncomfortable. The discomfort and severity of this might worsen over time, turning the eyes red. Use of hard contacts following eye surgery might also result in giant papillary conjunctivitis (GPC). Eye infections may be a result of improper handling of contact lenses, solutions, and cases.
4) Perennial conjunctivitis: All year round, perennial conjunctivitis. It primarily results from a dust mite allergy. These tiny, insect-like animals primarily inhabit carpets, upholstered furniture, and bed linens. Dust mites are attracted to warm, humid settings where they can feed on human skin cells. An immunological reaction to a particular dust mite protein causes dust-mite allergies. Conjunctivitis, a blocked or runny nose, sneezing, and tightness of the airways, similar to asthma, are just a few of the issues caused by this. Dander from animals, tiny scales from animal skin or hair, and bird feathers are some more reasons. Some people may develop an allergic reaction to them.
Diagnosis of allergic conjunctivitis:
In addition to checking your eyes, your doctor will go over your allergy history. Conjunctivitis can be seen as redness in the eye's white and little pimples inside your eyelids. One of the following tests may also be recommended by your doctor.:
1. An allergy skin test allows your doctor to study your body's reaction, which may include swelling and redness, by exposing your skin to specific allergens.
2. A blood test could reveal whether your body is making antibodies against particular allergens like dust or mold.
3. To check your white blood cells, a doctor may take a scrape of your conjunctival tissue. White blood cells called eosinophils are activated when you have allergies.
Complications of allergic conjunctivitis:
Perennial or seasonal allergic conjunctivitis rarely has complications. Although allergic conjunctivitis has a short-term influence on health, it can have a negative impact on a person's quality of life. Dermatoconjunctivitis and large papillary conjunctivitis can have complications. The cornea could swell up. This condition, referred to as keratitis, can result in corneal ulcers. This raises the potential of scarring and permanent eyesight loss.
The Symptoms of keratitis include:
a. excruciating eye pain.
b. light sensitivity.
c. vision haze.
d. a perception of something in the eye.
e. Eyes that are wet.
If these signs appear, the patient should visit a doctor.
Prevention of allergic conjunctivitis:
Avoiding environmental factors is the best approach to prevent allergic conjunctivitis, although this can be challenging. Depending on the cause, it might be beneficial if you:
a. exclusively make use of fragrance-free soaps and detergents.
B. add an air purifier to your residence.
c. routinely dust and hoover.
d. Keep your home's carpets, plush toys, drapes, and soft furnishings to a minimum.
Allergic conjunctivitis is a risk for whom?
Conjunctivitis caused by allergens is more likely to occur in allergy sufferers. In the United States, seasonal allergies affect 8% of adults and 7% of children, according to the Asthma and Allergy Foundation of America. You are more prone to allergic conjunctivitis if you reside in an area where high pollen counts are typical.
Keep in mind that while these steps offer broad advice, it is crucial to speak with a healthcare provider for a precise diagnosis and individualised treatment plan for your particular problem. Conjunctivitis that is allergic can develop after being exposed to allergens such as house dust or mold. Itching, redness, and watery eyes are symptoms. Avoiding the causes of the condition and using over-the-counter medications are two treatment options for allergic conjunctivitis. A doctor might recommend medication if these are ineffective.